About a year ago I fractured and dislocated my ankle. I was taken by ambulance to the Emergency Department at Boca Raton Regional Hospital. There I was examined, treated, sent to a hospital room and scheduled for surgery the next morning. Thankfully all went well. My orthopedic surgeon did a great job putting my ankle back together. That visit to the ER prompted me to do some research about ERs in our country.
Emergency rooms (ERs) also known as emergency departments, are critical access points within the American healthcare system that deliver urgent medical care 24/7. These facilities are designed to treat severe, life-threatening conditions, such as chest pains, major trauma, respiratory distress, and stroke. They also serve as safety-net providers for patients lacking primary care access or comprehensive insurance coverage. ERs function as both entry points for hospital admissions and wide-ranging care centers for urgent conditions when other options are unavailable.
The need for emergency care in Boca Raton has grown exponentially in recent years. Witness the large number of private emergency facilities such as “MD Now” which has over 100 locations in Florida. In addition, Boca Raton Regional Hospital recently opened a new emergency facility in West Boca Raton located in Mission Bay Plaza off Glades Road on Route 441. The 116,800-square-foot ER provides round-the-clock emergency services. “We are thrilled to expand our services in the West Boca community. We provide timely and expert care when every second counts,” said Ms. Batista-Rodriguez, CEO of Baptist Outpatient Services. The facility includes 18 exam room and a comprehensive diagnostic imaging services, including CT scans and x-rays. These services are available 24/7 making it a one-stop destination for urgent medical needs.

Emergency departments in the United States receive massive patient traffic. Statistics from the Center for Disease Control say ERs recorded 155 million visits in 2024, illustrating the enormous demand for emergency care. The national average ER visit rate in 2023 was approximately 422 visits for 1,000 population though this varies widely among the states. For example, Nevada averages 226 visits per 1,000 residents while West Virginia averages 596 patient visits per 1,000. Demographic patterns showed that children under 15 contribute to about 12% of all visits to ERs. Utilization rates are higher in urban areas compared to those in rural settings. While most patients are treated and released a subset requires hospital admission. Approximately 11.5% of ER visits result in subsequent hospital admission.
Triage – Bleeding, Breathing and Little Children go First
Today, a typical hospital has its emergency department in its own section of the ground floor, with its own dedicated entrance. Since patients can arrive at any time and with any problem, a key part of the operation of an emergency department is the prioritization of cases based on clinical need. This process is called Triage. Triage is normally the first stage the patient passes through, and consists of a brief assessment by a Triage nurse. It includes taking of a set of vital signs, and the assignment of a “priority condition.” For example, chest pain, abdominal pain, difficulty breathing, bleeding, etc.” Most emergency departments have a dedicated area for this process to take place, and often have staff dedicated to performing nothing but triage. In most ER departments this role is fulfilled by a triage nurse. A form of triage may also be conducted via radio with an EMT ambulance crew. In this method, the paramedics will call the hospital triage center providing a report regarding the status of the transported patient.
Most patients will be initially assessed at triage and then passed to another area of the ER department. However, some patients may complete their treatment at the triage stage. For example, if the condition of the patient is not very serious and can be treated quickly, no further action in the ER will be needed. Likewise, if only advice is required, or if the emergency department is not a suitable point of care for the patient, they may be discharged. Conversely, patient with evidently serious conditions, such as cardiac arrest will bypass triage altogether, and move straight to the appropriate part of the department.
The resuscitation area, commonly referred to as trauma is a key area in most ER departments. The most seriously ill or injured patients will be dealt with in this area, as it contains the equipment and staff required for dealing with immediate life-threatening illnesses and injuries. In such situations, the time in which the patient is treated is crucial. Typically, resuscitation staffing involves at least one attending physician, and at least one and or two nurses with trauma and Advanced Cardiac Life-Support training.
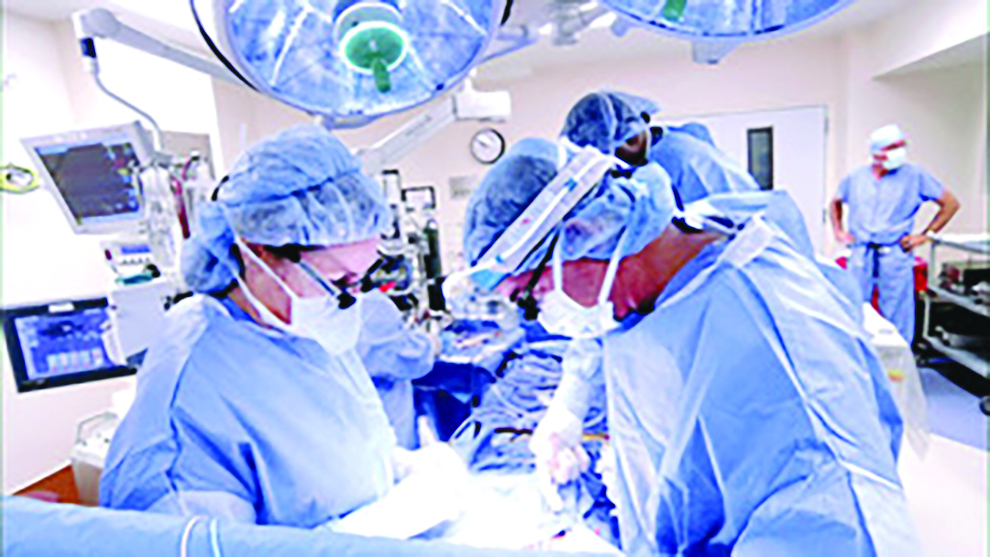
Patients who exhibit signs of being seriously ill but are not in immediate danger of life or limb, will be triaged to “acute” or “major” care where they will be seen by a physician and receive a more thorough assessment and treatment. Examples of “major” include chest pain, difficulty breathing, abdominal pain and neurological complaints. Advanced diagnostic testing may be conducted at this stage, including laboratory testing of blood, CAT scans or MRI scanning. Medications appropriate to manage the patient’s condition will also be given. Patients may be discharged home from this area or admitted to the hospital for further treatment, depending on underlying causes of the patient’s chief complaint.
The patients whose condition is not immediately life-threatening will usually be sent to an area suitable to deal with them, and these areas might typically be termed a “prompt care” or “minor” area. Such patients may still have been found to have significant problems, including fractures, dislocations, and lacerations requiring suturing. That’s where I went when I broke my ankle.
Special Cases
Rates of ER visits related to mental health concerns have been rapidly increasing. This puts additional strains on facilities not really designed for psychiatric care. These often include people who are actively a risk to themselves or others (e.g. suicidal). Some ERs have a separate area for evaluation of psychiatric problems. These are often staffed by hospital psychiatrists and mental health nurses and social workers.
Major Challenges facing ERs today
Waiting times
Waiting times in ERs remain a persistent problem. Nationally average wait times in emergency rooms vary from 30 minutes to 2 hours. The national median wait time is roughly 1 hour. This delay may in part be due to a shortage of primary care facilities or because many people cannot afford to go to a primary doctor or a private facility like “MD Now.” Going to the ER is often a last resort for those without the money or insurance to go elsewhere. It is estimated that 50 percent of the U.S. population fall into the group. Therefore, they rely on the ER for what is often primary care. Federal law forbids denial of care if the facility is a Medicare provider. That includes most regional hospitals. A major cause of delays is the fact that there is a shortage of primary doctors in our country. This gap is widening. New answers must be found, or the situation will progressively worsen.
ERs see a sharp mix of urgent and non-urgent cases. Most ER visits are not for immediate life-threatening conditions. Studies suggest that over 75 percent of cases are non-urgent and could potentially be managed in an out-patient settings. Visits related to abdominal or chest pain, infections, injuries and respiratory issues account for a large percentage of ER visits. Issues related to alcohol or drug abuse, homelessness, psychiatric issues, sunburn, pregnancy also cause visits to the ER.
Admission to Hospital from the ER
When the staff in the ER determine that a person needs to be admitted to the hospital, that patient is often referred to as a “boarder” while they are still in the ER. Boarding rates have increased nationwide. Often, patients may have to wait several hours for a room with a vacant bed to open up. Extended ER boarding creates bottlenecks, limiting capacity for new arrivals and contributing to overcrowding and delays. In Boca Raton, this problem will be reduced when the new “Gloria Drummond Patient Tower” opens later this year.
Cost of Emergency Care
If an uninsured patient shows up in the ER, who pays? The hospital? The taxpayers? The patient? Under the Affordable Care Act (Obama Care) hospitals provided about $40 billion in “uncompensated care.” That represented 6% of the hospital’s total expenses. A visit to an ER typically costs $1,500 to $3,000 for patients with minor issues. It will be much higher for those with serious problems. In 1985 a federal law requires ER departments to stabilize and treat anyone entering their doors, regardless of their ability to pay. Hospitals may not even ask if the person is insured. Note: There are 25.6 million uninsured, excluding elderIy, people in the U.S.A. Hospitals fortunately get help from taxpayers. They receive federal and state funding to offset some of the care for treating the poor. In 2023, Florida received almost $1 trillion from the Federal government for hospital and medical care for the needy. In July 2025 the Palm Beach County Commissioners also voted to allocate $300 million for health care for the needy. ERs are a great community resource. Residents of Boca Raton are very fortunate to have very good ERs. More information regarding Emergency Care is available on numerous websites and from your hospital of choice.